PANCREATITIS
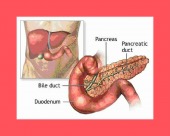
Pancreatitis is an inflammation or infection of the pancreas.
Early symptoms include nausea and abdominal pain.
Acute pancreatitis is often caused by gallstones obstructing the pancreatic duct. Digestive juices got backed up into the pancreas itself, where they attack healthy tissue and destroy cells that produce both enzymes and insulin.
Ongoing damage to enzyme-producing tissue in chronic pancreatitis leads to poor absorption (malabsorption) of nutrients, especially fats, to weight loss, and to oily, malodorous stools. And damage to or destruction of insulin-producing cells means blood sugar isn't metabolized properly, often leading to diabetes.
The other major contributor of acute pancreatitis is alcohol which causes digestive enzymes to be released sooner than normal. It also increases the permeability of the small ducts that convey enzymes within the pancreas, which allows digestive juices to leak into and damage healthy tissue. What's more, excessive alcohol intake leads to the formation of protein plugs — precursors to small stones — that block parts of the pancreatic duct.
Other factors that can cause or contribute to pancreatitis include:
- Increased blood levels of fats called trigylcerides (hyperlipidemia) or of calcium (hypercalcemia)
- Certain medications, including corticosteroids and nonsteroidal anti-inflammatory drugs, blood pressure lowering drugs (thiazides), antibiotics such as tetracyclines and sulfonamides, and medications that suppress the immune system such as azathioprine and 6-mercaptopurine. Drug-induced pancreatitis constitutes 2 to 5% of reported cases acute pancreatitis. People at risk of drug-induced pancreatitis include elderlies on multiple medications, HIV patients, patients on immunomodulatory agents.
- Viral infections (e.g. mumps, hepatitis)
- Bacterial infections
